As briefly mentioned in the previous post, I recently (in the last two years) starting experimenting with what it would be like to set goals in line with my desires. This seems basic as I type it, but I think what I was doing before was setting goals in line with my hopes or maybe more realistically, my shoulds. Even if it was a goal I wanted (desired) to accomplish, I would set it on a hope/should timeline. For example, I wanted to publish a book – by the time I was thirty – and I didn’t. Although really, I just meant that I wanted to write in a format that other people would read. But I thought I needed to manipulate this desire into a framework where I could measure it and check it off and somehow through that process feel good about it. I wanted to accomplish!
I’m 35 and I haven’t published a book. At the start of the pandemic I put together a manuscript of poems from my twenties and submitted it to a poetry publishing contest. I didn’t win and then I didn’t really pursue it further, in large part because the poems I had compiled didn’t speak to me the way they had years before. Almost all of my poems are about things that fly – birds, bugs, bats, that kind of thing. And searching for something. I guess maybe once I had gone off to find something else, these poems didn’t make as much sense to me as they once had.
The interesting thing about pursuing a sense of good feelings, aka accomplishment, through goals is that if you’re not careful, you’ll take the joy out of the process. I’ll never write a book by the time I’m 30. I’ve missed my goal. Should I even write? What’s it all even for?
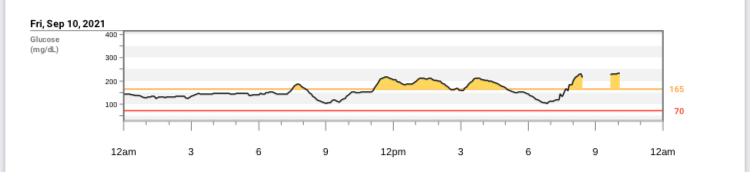
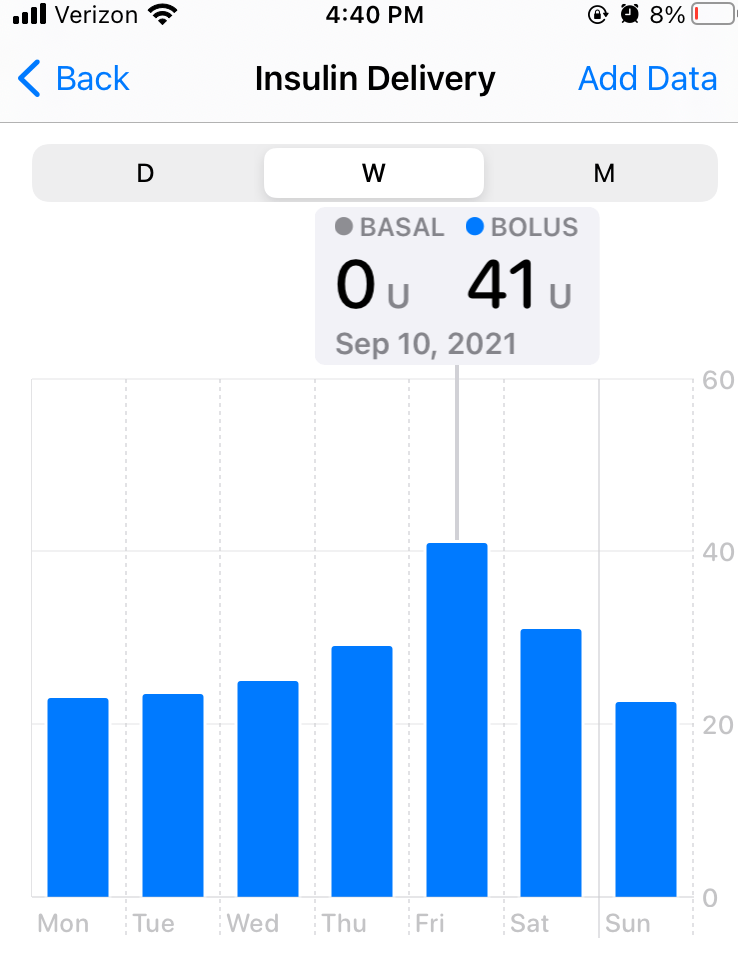
So that is why last year I set my New Year’s Resolution to eat more cheese. I knew I wanted cheese and I also knew I would eat cheese, and aren’t goals just about fulfilling our desires anyway? I have to tell you it went really well. I’m not saying I did this to make a big statement to myself, it was more of a joke, but I did notice that if flipped the script a little bit. When I was first diagnosed with diabetes I got a food scale. I was a freshman in college and had struggled with times of obsessing over calories in high school. Suddenly I was sanctioned to restrict my food (albeit based on carbohydrates, not calories) in the name of blood glucose management. While I actually did learn a lot about carbohydrate counting that has been beneficial for me throughout my time with diabetes, it also contributed to the culture of restriction I was building for myself around diabetes management. And chronic conditions rarely visit alone – so I amassed other restrictions and before long I was running into many invisible walls hoping that if I could just stay within them, I would feel great.
These last few years, maybe starting in the height of the pandemic, have been some of my least restricted when it comes to diabetes. And I’m happy with my current blood glucose ‘control,’ aka levels. I want to be clear that this doesn’t mean that I abandoned blood glucose targets or stopped counting carbs or bolusing when I eat or any of the other self-management tasks, it just means that I loosened my grip on achieving blood glucose perfection. Sometimes this meant that I rested instead of taking a walk. That I ate foods I would not have eaten at other points in my diabetes journey, just because others were having it and I wanted to share. That I didn’t feel bad about having to correct for it later. Sometimes I did still feel bad for it, but I didn’t let that stop me from making that brave choice. I loosened my grip on the idea that somehow, if you took everything else away, perfection was even something I had control over.
Because you can’t remove all the other variables from life. There are other goals in my life besides my hemoglobin A1c or time in range that are really important to me and that I want to prioritize. In fact, my motivation for glucose control is to live the life I desire, so constant restriction will never get me there. By the way, food is just an example, not the point here. The point is that there are ways I was trying to control the situation through any means I had available. And for certain aims, that control worked, especially at various points in my diabetes learning journey. But, now when I step back and ask, ‘why the control?’ I’m confronted with the desire to be more fully present with my life. My goals are flexible and interconnected. Maybe I’ll write a book, maybe not. In the moment, other things might feel more important, like making plans with friends or taking a last minute trip with my mom, or doing nothing with a cup of tea.
*This blog contains my personal reflections on my journey only. I am not a medical provider and nothing in this blog is intended to serve as medical advice.